T Cell Selection and Maintenance
By Jason Socrates
Bardi
"Am
not I
A fly like thee?
Or art not thou
A man like me?"
———William
Blake, Songs of Innocence and of Experience
Insects rely solely on innate immunity to recognize and
fight off foreign infections, but unlike insects, humans have
a second part to their immune system, known as adaptive immunity.
"The adaptive immune system counters infectious agents,"
says The Scripps Research Institute (TSRI) Professor Jon Sprent.
"It [reduces our] susceptibility to infection."
Sprent and his colleague in TSRI's Department of Immunology,
Associate Professor Charles Surh, have been studying for a
number of years the cells that act as crucial mediators of
this adaptive immune response.
The adaptive immune response is slower than the innate,
but it has a much higher—indeed, exquisite—specificity.
Acquired immune response cells are able to recognize almost
unlimited shapes and forms of pathogens with such discrimination
that they can tell the difference between peptides that vary
by only a single amino acid.
Cells of the adaptive immune system are able to do this
because they are, as a population, extremely diverse. The
basic strategy of the adaptive immune system is to make as
many receptors as the body is able, but to keep the number
of cells low. The body sacrifices population for the sake
of diversity, so that there will only be a few cells that
can respond well to any particular insult.
This explains one of the chief differences between the adaptive
and the innate immune systems: speed of response. The few
cells that do specifically recognize some part of a pathogenic
invader need time to multiply before they can mount a response.
And multiply they do—in abundance. A single T cell, one
of two key players in the adaptive immune response, can proliferate
into a million cells in a matter of days once it has been
activated.
T of Edward's Cells the Murderer Shall Be
T cells, so named because they are created in the thymus,
are the focus of Sprent and Surh's studies. Their long-term
goal is to understand how to counter diseases and, perhaps,
come up with better and more effective vaccines. They are
particularly interested in the development of the T cells
in the thymus and in how they are maintained in the peripheral
lymphoid tissues.
Development in the thymus occurs through a highly sophisticated
mechanism whereby the thymus sorts out those cells that are
potentially useful in the periphery from those that are not.
This is achieved by screening the cells for their binding
affinity for major histocompatibility complex (MHC) molecules,
the receptors that are present on antigen-presenting cells
recognized by the T cells' own receptors. For mature T cells
in the bloodstream, antigen-presenting cells display pieces
of pathogenic invaders (antigens) in their MHC receptors,
and this leads to the activation of T cells that have the
right receptor—one that binds that antigen-loaded MHC
tightly.
In the thymus, MHC molecules also play a crucial role, so
they must be recognized by the T cells. However, the purpose
of this recognition is not to activate the T cells, but to
select among them based on the results of the screening. Only
a small percentage survive.
"Well over 95 percent of the T-cells that are made in the
thymus are destroyed there," says Sprent.
Negative and Positive Selection
T cells are meant to recognize bacterial or viral structures,
but the test for developing T cells in the thymus is recognizing
MHC that is loaded with "self" antigen. Through two separate
selections, the thymus selects T cells that recognize this
self antigen—but weakly—and releases them into the
periphery.
Most developing T cells don't bind to MHC at all, and these
are selected for programmed cell death. Of the remaining cells,
those that have been positively selected for their ability
to recognize self antigen, a further selection takes place.
Those that are highly reactive are selected to die as well.
The elimination of these highly reactive T cells is called
negative selection or central tolerance, and is an important
complement to the positive selection because of the volatility
of these highly reactive T cells.
"If these cells were allowed to get out of the thymus, they'd
attack all our self-components," says Sprent. "We'd turn into
a giant kidney allograft."
Cells that recognize self antigen with low affinity are
allowed to live and trickle through to the periphery, where
they circulate as mature T cells. They do not, however, go
on to attack self tissue weakly just because they recognize
it with low affinity. Once T cells are outside the thymus,
they are long-lived and circulate while awaiting signals to
activate them—during an immune response to a viral infection,
for instance.
Though only a small percentage of the total number of T
cells made in the thymus are released, the thymus makes a
huge number of T cells, so the pool of T cells in the periphery
is still large.
This large pool is important to the body's ability to respond
to any insult from a foreign pathogen. The body's diversity
of T cells, some of which will have receptors that recognize
molecular components—antigens—of the pathogen with
high affinity, will mediate an immune response upon encountering
those antigens.
Activated T cells fall into two categories. Helper T cells,
sometimes called CD4+ T cells because they display the CD4
protein on their surface, secrete chemicals that activate
the body's other major class of adaptive immune cell, the
B cells. Cytotoxic, "killer" T cells, which are distinguished
by the CD8 protein they display, are responsible for destroying
cells that are infected with pathogens by inducing apoptosis,
or programmed cell death, in those infected cells.
In either case, a range of T cells will recognize any one
structure of foreign pathogen. However, only those T cells
that bind with high affinity, or with great preference, to
antigen presented in MHC will become activated "effector"
cells.
"There is a threshold of affinity that a T cell requires
in order to make a response," says Surh. "In order to become
a killer, the cell must be engaged at that high affinity."
1 | 2 |

|

Investigators Jon Sprent and Charles
Surh study T cells, with the long-term goal of understanding
how to counter diseases and, perhaps, come up with better
and more effective vaccines. Photo
by Jason S. Bardi.
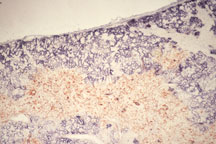
Depiction of distinct populations of
epithelial cells in the mouse thymus. Cortical epithelial
cells (blue) mediate positive selection of immature thymocytes.
Selected thymocytes then enter the medulla, the site where
different populations of epithelial cells (including one which
is stained red) exist; some of these populations mediate negative
selection to eliminate thymocytes that are overtly-reactive
to self antigens. The exact function of the medullary epithelial
cells stained in red is not known. (Double staining was performed
on frozen sections of normal B6 adult thymus using 6C3 and
anti-H2-O antibodies.)
|

