|
(Page 2 of 2)
Activation of the coagulation cascade generates thrombin.
Thrombin is a very efficient proteolytic enzyme—it cleaves
other proteins at specific points in their amino acid sequences.
One of the proteins it cleaves is fibrinogen, which makes
fibrin, the sticky, clot-forming protein. Thrombin also cleaves
receptor proteins displayed on cell surfaces, which then "transduce"
a signal inside the cell. The first of such a receptor identified
was the thrombin receptor or protease activated receptor 1
(PAR1), a receptor of the broad class of G protein-coupled
receptors. The activation of this receptor on platelets is
critical for platelet activation and hemostasis.
Like all coagulation factors, thrombin circulates as a zymogen—an
inactive precursor. If the body needs to make use of thrombin
for the clotting cascade, for instance, it must first activate
the zymogen "prothrombin" by clipping off the "pro-" part
to get thrombin. Obviously, this action must be tightly controlled
by the body to avoid causing blood clots willy-nilly. One
of the ways the body accomplishes this is by requiring prothrombin
to associate with other molecules—called cofactors—before
it can be processed into its mature form. The body uses other
enzymes to control the cofactors and activated protein C is
the enzyme that inactivates the prothrombin cofactor. Activated
protein C, thus, in an indirect way controls blood clotting.
Activated protein C is itself normally present as a zymogen,
called protein C, and it only becomes active when it is cleaved
into its active form. Interestingly, thrombin is the molecule
responsible for activating protein C. Thus the two work together
in a feedback loop to balance each other, thrombin activating
the protein C, which deactivates the cofactors that make thrombin,
which reduces the amount of activated protein C, and so on.
This balance is important for maintaining good health and
the feedback loop that generates activated protein C occurs
on the surface of endothelial cells. Endothelial cells are
one of the major cell types of the body, accounting for about
one percent of the total cells in the body. They line all
blood vessels and capillaries and contribute to the structural
integrity of the circulatory system.
Once endothelial cells go, big problems arise—when
endothelial cells suffer widespread damage, organs can fail.
The Mystery Solved
Inactive protein C binds to a specific receptor on the surfaces
of these endothelial cells—called endothelial cell protein
C receptor (EPCR). There, the inactive protein C can be activated
by thrombin. To do so, thrombin needs to bind to another endothelial
cell receptor, termed thrombomodulin. When thrombin is bound
to thrombomodulin, thrombin looses all its clotting function
and solely serves to activate the protein C pathway. In sepsis,
the physiological balance between thrombin and activated protein
C is lost, because inflammatory cytokines cause a loss of
thrombomodulin from endothelial cells. Thrombin can no longer
activate protein C, and without activated protein C, the endothelial
cells cannot be protected.
Ruf and his colleagues have now shown that ECPR is also
required for activated protein C to trigger a cascade that
upregulate genes that prevent apoptosis, or programmed cell
death, and genes that downregulate inflammation and protect
these endothelial cells from damage.
Surprisingly, this cascade involves the thrombin receptor
PAR1. PAR1 was the missing link between the activated protein
C and its protective effect on endothelial cells. Clinical
trials had established that endothelial cells can be protected
by activated protein C during sepsis, but nobody knew how.
Ruf and his colleagues demonstrated that activated protein
C protected these endothelial cells through PAR1 signaling
by asking whether the genes that the activated protein C induced
could be accounted for by the activation of the PAR1 receptor.
They ran gene profiling using gene chip microarrays, which
allowed them to look on a genome-wide scale, and they found
about 100 genes that are reproducibly turned on by PAR1. Then
they compared those to all the protective genes that are upregulated
by activated protein C, and they found that they could all
be accounted for by the activation of the PAR1 receptor.
Thus, the mystery was solved. Thrombin binds to thrombomodulin
on the surface of endothelial cells and activates the nearby
protein C bound to the EPCR. And activated protein C will
then activate the PAR1 receptor.
However, Ruf and his colleagues also found a few genes that
were upregulated by PAR1 signaling, but not by the signaling
of activated protein C. Some of these genes may explain why
thrombin has inflammatory effects, while activated protein
C is protective and beneficial. One current direction of the
laboratory is to determine what combinations of gene upregulations
confer protection or cause damage of endothelial cells
The article, "Activation of Endothelial Cell Protease Activated
Receptor 1 by the Protein C Pathway" was authored by Matthias
Riewald, Ramona J.Petrovan, Aaron Donner, Barbara M. Mueller,
and Wolfram Ruf and appeared in the June 7, 2002 issue of
the journal Science.
1 | 2 |

|
When Endothelial Cells See Thrombin
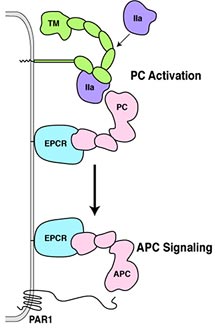
In the top panel, inactive protein
C (pink) associates with the EPCR receptor (blue) on the surface
of an endothelial cell. Thrombin (purple), which is drawn
to thrombomodulin (green), activates protein C. The consequence
of this, shown in the bottom panel, is that activated protein
C will then activate the PAR1 receptor.
|

