

Team Finds a Widely Used Anti-Malarial Drug Prevents Cancer Development
By Eric Sauter
Scientists at The Scripps Research Institute and St. Jude's Children's Research Hospital have found that a commonly prescribed anti-malarial drug effectively prevents the development of certain types of human cancer in mouse models.
The drug, chloroquine, which has been in use since 1946, prevented development of cancer in models of two distinct human cancer syndromes, Burkitt lymphoma, a cancer of the lymphatic system, and ataxia telangiectasia (A-T), a rare and progressive immunodeficiency disease that predisposes patients to cancer, especially lymphoma and leukemia.
The study was published in an advance online edition of The Journal of Clinical Investigation on December 20, 2007. It appears in the journal's January 2008 edition.
"Our study shows that chloroquine inhibits the final steps of a pathway that is required for tumor cell survival and effectively eliminates cancer cells in mouse models that replicate human tumors," said John Cleveland, a Scripps Research scientist who is chair of the Department of Cancer Biology at the institute's Jupiter, Florida, campus. "The fact that the drug attacks premalignant cells, and cells that overexpress transcription factor MYC, a notorious contributor to tumorigenesis that is implicated in more than 70 percent of all cancers, makes the use of this drug very attractive for chemoprevention and cancer treatment."
In the study, chloroquine was very effective in delaying the onset of spontaneous tumors in mice lacking ATM. The ATM gene is akey arbiter of the DNA damage response pathway and is mutated in patients with the cancer-inducing disorder ataxia telangiectasia. These malignancies are particularly difficult to treat because of the acute sensitivities of A-T patients to cytotoxic agents. Chloroquine now offers a potentially novel treatment for these patients because the drug preferentially eliminates cancer cells and is relatively well tolerated.
In addition, the scientists found that treating mouse models of human Burkitt lymphoma just once every five days also dramatically reduced lymphoma development. Interestingly, an epidemiologic study completed in the 1980s supports the potential of this treatment in humans. While this study was designed to investigate the link between malaria and the high incidence of Burkitt lymphoma in equatorial Africa, researchers found that chloroquine treatment decreased the incidence of lymphoma in the region by about 75 percent.
The Mechanism of Cancer Prevention
Exploring the mechanism of the drug's cancer-preventing action provided some intriguing insights.
At the doses used in the new study, which were similar to those needed to prevent malaria, chloroquine triggered the death of premalignant cells. This suggests that within the context of MYC overexpression, the drug induces apoptotic cell death—programmed cell death—in response to ineffective autophagic protein degradation and lysosomal changes in the cell. (Lysosomes are cellular recycling centers that degrade old and unwanted material in the cell and recycle building blocks that are used for cell growth.) The p53 protein can induce apoptosis in response to DNA damage or stress, and the study's results suggest that alterations in lysosomal function trigger a p53-dependent cell death response.
"Our studies have established that chloroquine inhibits a late step in the autophagy pathway by inhibiting lysosome functions that provide necessary material used to keep tumor cells alive under times of stress," Cleveland said. "Autophagy is also triggered by starvation, which is common in rapidly dividing tumors. Compounds like chloroquine derail this response and enable the body to effectively clear tumor cells."
Autophagy is a complex adaptive cellular response that enhances cell survival in the face of starvation or other stresses, including protein accumulation in the cell. Other recent studies from the Cleveland lab suggest that drugs that disable the autophagy response can overcome treatment resistance, even in refractory tumors.
While the new study shows that chloroquine's disruption of lysosomal function makes it potentially useful in the treatment of certain cancers, there are still questions to be answered before the treatment arrives in the clinic. The team is working on defining the optimal use of this approach for cancer prevention and treatment. Issues include dosing, particularly in combination with other agents that are used to treat cancer patients.
"The most important fact is that our study provides proof of principle for developing antitumor therapies based on the modulation of autophagic pathways," said Cleveland, "and this offers multiple opportunities for novel drug discovery, whether based on chloroquine or targeting other steps in the autophagy pathway."
In addition to Cleveland, authors of the study, Targeting Lysosomal Degradation Induces p53-Dependent Cell Death And Prevents Cancer In Mouse Models Of Lymphomagenesis, are Kirsteen H. Maclean and Michael B. Kastan of St. Jude Children's Research Hospital, and Frank C. Dorsey of The Scripps Research Institute.
The study was supported by the National Cancer Institute, the Cancer Center (CORE), and the American Lebanese Syrian Associated Charities of St. Jude's Children's Research Hospital.
Send comments to: mikaono[at]scripps.edu
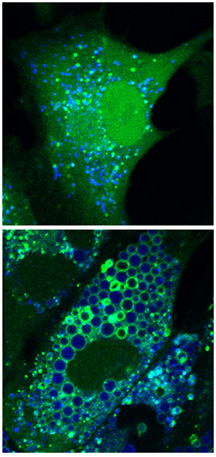
Scientists have found that the drug chloroquine, which has been in use since 1946, can prevent development of cancer in models of two distinct human cancer syndromes. The above images show the contrast between cells that are untreated (top panel) and those that are treated with chloroquine for just four hours (bottom panel). Autophagosomes are shown in green; lysosomes, in blue. Note the massive accumulation of large, dysfunctional lysosomes that precedes cell death in chloroquine-treated cells.
