

To Stop Evolution:
Scientists Demonstrate New Way of Fighting Antibiotic Resistance
By Jason Socrates Bardi
A team of scientists at The Scripps Research Institute and the University of Wisconsin has demonstrated a new way of fighting antibiotic resistance: by stopping evolution.
In the June issue of the open-access journal PloS Biology, the team describes how a protein called LexA in the bacterium Escherichia coli promotes mutations and helps the pathogen evolve resistance to antibiotics. The scientists also show that E. coli evolution could be halted in its tracks by subjecting the bacteria to compounds that block LexA. Interfering with this protein renders the bacteria unable to evolve resistance to the common antibiotics ciprofloxacin and rifampicin.
"If you inhibit this pathway, the bacteria cannot evolve," says Scripps Research Assistant Professor Floyd Romesberg, who led the study.
Since the evolution of resistance is under the control of LexA, compounds that block the protein might prolong the potency of existing antibiotics.
Evolution—It's not Like Death and Taxes Anymore
This research raises fundamental questions about evolution. Biologists have often thought about evolution in the same way many think about death and taxes—something inevitable. But Romesberg is a chemist, and he found himself asking not only how, but why evolution happens.
For the last few years, Romesberg has led an effort to understand the genes that drive evolution, an innovative way of thinking because scientists have more often understood evolution as the force that drives genes. What underlies evolution is mutation—changes in the DNA. "Mutations are the fuel for evolution," says Romesberg.
Because of the potential harm of mutations, humans and other mammals have evolved to make as few as possible. The machinery inside our cells has the ability to replicate our genomes extremely well, and the "polymerase" enzymes that replicate our DNA rarely make mistakes. Even when they do, we have multiple, redundant repair and proofreading mechanisms that would make even the most six-sigma-compliant NASA engineer jealous.
Nevertheless, all organisms are prone to some level of damage because no replication machinery is perfect, and with large genomes of billions of bases of DNA to be copied many billions of times over the lifetime of an organism, a certain level of spontaneous mutations will occur—mistakes that escape repair and become part of the DNA of the cell in which they occur. Scientists have generally thought that slowly over time, these mutations accumulate and species diverge.
However, Romesberg and his colleagues believe that cells are not just the passive victims of random mutations, but have ways of initiating mutations in their own DNA. Evidence for this includes the fact that the rates of mutation in some cells does not seem consistent with the mutation rates associated with DNA replication.
Some cells, like bacteria subjected to antibiotics, seem to acquire mutations at a much higher rate. Romesberg reasons that these rapid mutations may sometimes be part of a mechanism organisms have to rapidly evolve when they need to.
Stress and Mutations
A few years ago, when he was first starting to think about this, Romesberg encountered a paper in a scientific journal that discussed certain genes that "make mutations," as he put it. When these genes are deleted from cells, the cells lose their ability to mutate, even when subjected to massive amounts of ultraviolet light.
This brought Romesberg to the conclusion that mutation is a programmed stress response—a survival mechanism. If the cell senses damage, and if the damage persists beyond its ability to repair it, the cell will turn on its mutation machinery and open the floodgates for evolution.
Take the bacterium Escherichia coli for instance. When E. coli cells are subjected to damage, they upregulate repair enzymes, which then go to work trying to fix the problem. If the damage persists, the cell upregulates recombination enzymes, which are tasked with recombining the DNA—another way to repair it. And, says Romesberg, if the damage still persists, the cells upregulate enzymes whose sole task is to make mutations.
Presumably, inducing mutations is an effective evolutionary strategy for dealing with environmental changes that maximize the chances that a progeny cell will be better adapted. In order to evolve, organisms have to mutate, so they turn on the mutation process when they are threatened with extinction.
Romesberg reasoned that since mutations can be turned on full-force, perhaps they could be shut off as well. Doing so, he says, would put a halt to evolution—an interesting prospect because the mutations responsible for evolution are the underlying causes of cancer and aging as well.
"Evolution is not an unstoppable force," says Romesberg. "There is a biochemistry underlying it and it is subject to intervention."
The Scourge of Antibiotic Resistance
One thing that scientists would like to change about bacteria and cancer cells is their changeability.
At the dawn of the 20th century, bacterial infections accounted for several of the leading causes of death in the United States. But then came the antibiotic revolution. Antibiotic "wonder drugs" toppled tuberculosis (TB) and typhoid fever, controlled cholera and gonorrhea, reduced staphylococcal dysentery, and lowered the incidence of many other pandemic bacterial infections. These antibiotics are basically natural chemicals (or derivatives of natural chemicals) produced by other bacteria or fungi in the environment to kill off the competition. Scientists in the last century have discovered a number of these natural "antibiotic" products and have used them as the basis for treating bacterial infections.
By the middle of the century, the threat posed by many types of bacteria seemed to be waning. Bacterial infections that once topped the list as leading causes of death in the United States were no longer among the top ten. The average life expectancy in the United States soared from 47.3 years in 1900 to almost 80 years today, and antibiotics are partly to thank for this.
But in the last few decades, mutant strains of several types of bacteria with the ability to resist antibiotics have emerged, including those that cause TB, pneumonia, cholera, typhoid, salmonella, and staphylococcal dysentery. These diseases are coming back resistant to the antibiotics that have been used to treat them, and people infected with these resistant strains have to be treated with alternative antibiotics. For years scientists have been combating drug resistance by coming up with new types of antibiotics, and for years bacteria have been evolving ways around these antibiotics.
Antibiotic resistance is a major health problem in the United States. According to the U.S. Food and Drug Administration (FDA), about 70 percent of bacteria that cause infections in hospitals are resistant to at least one antibiotic, and some are so resistant that no antibiotics are effective, and they must be treated with experimental and potentially toxic drugs.
Now some super bugs—multiple drug-resistant bacteria—are emerging as an even greater threat. Multiple drug-resistant TB is no longer susceptible to broad categories of antibiotics, such as rifampicin, isoniazid, and streptomycin. Some strains of the common hospital infection-causing bacteria Staphylococcus aureus are resistant to all antibiotics except vancomycin, which is a drug of last resort, and some strains of Streptococcus pneumoniae are even resistant to vancomycin. Certain strains of Shigella dysenteriae, the cause of epidemic dysentery, have even become resistant to all but a single drug—the quinolone ciprofloxacin—and may soon become completely untreatable. This is a major concern for public health because, according to the World Health Organization (WHO), large-scale epidemics of dysentery driven by this pathogen have been known to cause tens of thousands of deaths in Central America, South Asia, and central and southern Africa.
Treating multiple drug-resistant bacterial infections can be a hundred times more expensive than treating normal infections, and the WHO estimates the total cost of treating all hospital-borne antibiotic resistant bacterial infections is around $10 billion a year. Worse, with modern rapid transit and world travel, multiple drug-resistant bacteria could potentially spread beyond the isolated confines of a hospital and into the general population.
If one could design drugs to halt the enzymes that make mutations in bacteria, this could be a way of combating the evolution of antibiotic resistance.
The Dramatic Effect of LexA Inhibition
Halting evolution is exactly what Romesberg and his colleagues demonstrated in their latest PloS paper. They showed that when E. coli cells were treated with the antibiotics ciprofloxacin and rifampicin, they turned on their mutation pathways and rapidly evolved resistance to the antibiotics. Wanting to find the proteins that turn on the mutations, Romesberg and his colleagues identified a master regulatory switch that, if inhibited, blocks the ability of the cells to mutate.
This was the protein LexA, which belongs to the class of signaling enzymes known as serine proteases and works by cutting the amino acid chain of other proteins. Romesberg and his colleagues showed that LexA's action was necessary for the evolution of resistance to the antibiotics in vitro.
The effect in vivo was dramatic. Blocking LexA in rodent models of E. coli infections halted the growth of antibiotic resistance. Three days after being subjected to antibiotics, the rodents showed no level of resistance to rifampicin or ciprofloxin, when they harbored a variant of LexA that was catalytically inactive. In control experiments, the rodents were given rifampicin or ciprofloxin, and the scientists found that nearly all the wild-type E. coli cells had grown fully resistant to the antibiotics after three days.
This research is also significant for cancer because cancer cells mutate readily and often acquire resistance to common chemotherapies. Romesberg hopes that if he and his colleagues can identify the molecules that human cancer cells use to drive evolution, they can find ways of intervening and preventing the evolution of chemotherapy resistance in these cancer cells. Last year Romesberg was awarded a Department of Defense Breast Cancer Research Program Idea Award of $563,100 to identify the genes in Saccharomyces cerevisiae yeast and human cells that induce mutations that can transform normal cells into cancer cells.
The article, "Inhibition of Mutation and Combating the Evolution of Antibiotic Resistance" by Ryan T. Cirz, Jodie K. Chin, David R. Andes, Valérie de Crécy-Lagard, William A. Craig, and Floyd E. Romesberg appears in the June, 2005 issue of the journal PloS Biology. See: http://dx.doi.org/10.1371/journal.pbio.0030176
This work was supported by the Office of Naval Research.
Send comments to: jasonb@scripps.edu

For the last few years, Assistant Professor Floyd Romesberg has led an effort to understand the genes that drive evolution. Photo by Jason S. Bardi.
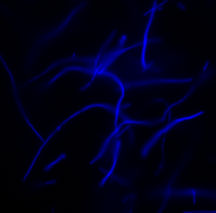 E. coli cells exposed to the antibiotic ciprofloxacin, with their DNA visualized with the nucleic acid binding dye DAPI. The image shows extensive elongation of the cells (they are normally short rods) as the antibiotic prevents normal DNA replication. Normally, the cells would quickly acquire resistance-conferring mutations and return to normal.
E. coli cells exposed to the antibiotic ciprofloxacin, with their DNA visualized with the nucleic acid binding dye DAPI. The image shows extensive elongation of the cells (they are normally short rods) as the antibiotic prevents normal DNA replication. Normally, the cells would quickly acquire resistance-conferring mutations and return to normal.
