

A Skin Cell Revisited
By Jason Socrates Bardi
The most seemingly unrelated chronic human health problems—asthma, psoriasis, and ulcerative colitis—share a root cause: inflammatory distress of the "epithelial" tissues, the thin layer of cells that makes up the outermost layers of skin and lines organs such as the intestines and lungs.
In recent years, scientists at The Scripps Research Institute and elsewhere have come to understand more about inflammation, disease, and the epithelial tissues, especially the role of a mysterious type of immune cell that resides mainly in these epithelial tissues called the gd T cell (pronounced "gamma–delta"). For years, scientists had postulated various biological roles for gd T cells, but aside from uncovering how they arise early in fetal development and then migrate to epithelial tissues, little was known about what these cells did—let alone about how they might be involved in disease.
Then about three years ago, Associate Professor Wendy Havran and her colleagues in The Scripps Research Institute Department of Immunology identified the first major biological role of the gd T cell—promoting wound repair. Now, in an article recently published online by the journal Nature Immunology, Havran and her colleagues Senior Research Associate Julie Jameson and former Research Associate Leslie Sharp and are reporting the details of how the gd T cells do this.
Standing Under the Skin
Prior to the paper three years ago, the more that had been discovered about gd T cells, the weirder they seemed. They were unlike the more familiar "white blood" T cells of the immune system (designated ab rather than gd) except that both arise in the thymus. Unlike regular T cells, the thymus nearly shuts off production of gd T cells later in development, most gd T cells do not circulate through the bloodstream, and the gd T cells in the skin seem to have little, if any, diversity and display a uniform receptor and recognize only a single antigen.
In the skin, gd T cells have a spiny, stretched-out, finger-like shape that contacts as many skin cells as possible. The cells they contact are mainly keratinocytes, the major type of epithelial cell in the epidermis—the outermost layer of skin. Keratinocytes are a profligate cell and are constantly dividing on the inner side of the epidermis, and the skin is constantly being renewed by this proliferation. As the keratinocytes move to the outer side of the skin, they become terminally differentiated and later undergo apoptosis (programmed cell death)—eventually to slough off into dust.
Havran, Jameson, and their colleagues’ big breakthrough came a few years ago when they were asking what role gd T cells play in the epidermis and discovered that the cells are a crucial mediator of wound healing.
When skin is cut or damaged, keratinocytes must proliferate to fill in the wound. And keratinocytes, they found, are able to faster re-epithelialize tissue that has been wounded if they can get help from the gd T cells.
In the study, Havran and Jameson compared knockout mice that lack gd T cells, to normal mice. "When gd T cells are missing, you see a delay in wound repair," says Havran. The mice also have problems with tumor rejection and have other skin problems.
Havran and Jameson postulated that the keratinocytes, sensing the damage, release an antigen that is recognized by the gd T cells, which then become activated. Once activated, the gd T cells undergo a morphological change and become little round factories. These begin mass-producing a growth factor that binds to keratinocytes and other epithelial cells, helping them proliferate and leading to the closure of the wound. The gd T cells also proliferate, multiplying to increase the response to the wound.
Solving the mystery of what the gd T cells are doing did not give Havran and Jameson all the answers, however. They did not know the identity of the antigen the gd T cells recognize. They also did not know the mechanism leading to the morphological change that starts the production of the keratinocyte growth factor.
Nor did they know whether the gd T cells played a role in the normal growth processes—since, after all, kertatinocytes are constantly undergoing proliferation and apoptosis in the epithelium.
So in the last couple of years, Havran, Jameson, and Sharp reexamined the mice that lack gd T cells.
Stopping Programmed Cell Death
They found that the keratinocytes in mice lacking gd T cells showed elevated levels of apoptosis.
Following this discovery, they reasoned that the gd T cells must produce some growth factor to protect the keratinocytes and that without gd T cells, the keratinocytes were not getting enough stimulation.
They then identified the growth factor that gd T cells produce—a small protein called insulin-like growth factor 1 manufactured mainly in the liver. Insulin-like growth factor 1 was previously known to play a major role in the homeostasis and apoptosis of cells in a number of tissues.
Havran, Jameson, and Sharp then demonstrated that this critical growth factor is important for stimulating keratinocyte growth, making these cells resistant to apoptosis, and maintaining keratinocyte homeostasis and skin barrier function.
The investigators showed that normal keratinocyte homeostasis in mice without the gd T cells could be restored by adding back in the recombinant insulin-like growth factor 1. The scientists made an equivalent rescue by adding the gd T cells directly.
They also showed that gd T cells undergoing a wound healing response produce increased amounts of insulin-like growth factor 1 and that this, not surprisingly, aids in the wound healing.
Quite apart from the basic science, Havran, Jameson, and Sharp's findings should be of interest to doctors who treat diseases that arise from epithelial cell disorders. These findings may eventually lead to the discovery of chemical compounds that could be used to treat conditions like psoriasis, ulcerative colitis, and asthma. Knowing the role of these cells in the skin and the mechanism whereby they interact with other skin cells may yield new potential targets for intervention in all of these conditions.
Havran, Jameson, and Sharp's findings may also be relevant to certain types of cancer because gd T cells are cytotoxic and have the ability to kill tumor cells.
The article, “Dendritic epidermal T cells regulate skin homeostasis through local production of insulin-like growth factor 1” by Leslie L Sharp, Julie M Jameson, Gabrielle Cauvi, and Wendy L Havran was published online by the journal Nature Immunology on December 12, 2004. See: http://www.nature.com/cgi-taf/DynaPage.taf?file=/ni/journal/v6/n1/full/ni1152.html
Send comments to: jasonb@scripps.edu

Associate Professor Wendy Havran and her colleagues recently published an article in the journal Nature Immunology.
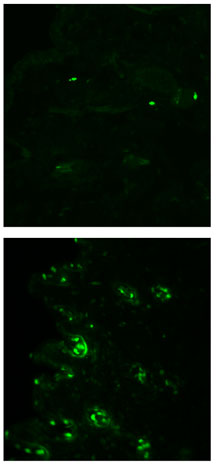
Cells within skin that is deficient in gamma delta T cells show increased levels of apoptosis. Dramatic proof of this can be seen in these fluorescent TUNEL assays: the green staining represents cells undergoing apoptosis, and a sample of skin from a wild-type mouse (top) shows relatively few apoptotic cells compared to skin from a knockout mouse (bottom). Image by Leslie Sharp.
