

Detecting the Genes That Contribute to Transplant Rejection
By Jason Socrates Bardi
La Jolla, CA, November 19, 2004—A group of physicians and scientists led by Associate Professor Daniel Salomon, M.D., of the Department of Molecular and Experimental Medicine at The Scripps Research Institute, has been awarded a new federal research grant of more than $12 million over five years to apply cutting-edge genomic technologies to advance our understanding of kidney transplantation. The grant was funded by the National Institute of Allergy and Infectious Diseases (NIAID), part of the National Institutes of Health (NIH).
Under the auspices of this program project grant, titled "Genomics for Kidney Transplantation," Salomon and his colleagues will monitor several hundred patients who have had kidney transplant surgeries with technologies for gene expression profiling and proteomics, and several thousand transplant patients by complex trait genetics (for descriptions, see below).
One of the team's overall goals is to answer one of the most pressing problems in kidney transplantation: why do some patients do well after a transplant while others do not?
"Fifty percent of transplant patients lose their kidneys within eight to ten years," says Salomon. "[This project] will study some 2,400 patients with kidney transplants, and we will be looking at the genetic basis and control of why some patients do well and others have problems. In practical terms, this will involve advancing our understanding of what causes acute and chronic kidney injury."
In addition to his laboratory research work, Salomon is also a transplant physician, Co-Director of the Scripps Health Center for Organ and Cell Transplantation at Scripps Green Hospital in La Jolla and Co-Director of the Scripps Research General Clinical Research Center's DNA Microarray Core—where some of the work on this project will be performed. Along with Salomon, the Transplant Genomics Collaborative Group includes Scripps Research Cell Biology Professor John Yates, and Steve Head, who is the director of the Scripps Research DNA Array Core Facility, among others. A key role in the clinical program will be played by Christopher Marsh, Director of Transplantation Surgery and Co-Director of the Scripps Health Center for Organ and Cell Transplantation at Scripps Green Hospital in La Jolla. Other investigators on the grant include Steve Horvath, an assistant professor of human genetics and biostatistics and Director of the Array Data Analysis Group at the University of California, Los Angeles; Pui-Yan Kwok, the Henry Bachrach Distinguished Professor of the Cardiovascular Research Institute Faculty Director of the Genomics Core Facility at the University of California, San Francisco; Janet Warrington, Vice President for Emerging Markets and Molecular Diagnostics Research and Development at Affymetrix, Inc.; and Stuart Flechner, Director, Kidney Transplantation Program at The Cleveland Clinic.
Kidney Function and Failure
Kidneys are the organs within the human body that filter waste from the blood and produce urine. They also secrete certain hormones into the blood that the body needs to maintain a normal blood count, chemical balance and blood pressure. A person's kidneys are workhorses, filtering all the body's blood every 22 minutes and maintaining the blood's pH, salt concentration, and pressure.
Kidney dysfunction is common to many different disease states, including diabetes and hypertension, which can damage the tiny blood vessels within the kidneys. Several genetic and autoimmune diseases as well as bacterial and viral infections and environmental toxins can also cause progressive damage to the kidneys.
Regardless of the cause, severe damage can lead to kidney failure. Without functioning kidneys, a person cannot survive for more than a few weeks. People with significant kidney dysfunction are usually treated with dialysis, where blood is filtered through an external machine that does the job the kidneys would normally perform.
Another way to treat kidney failure is to replace a person's failed kidneys with a donated kidney. Since the first whole organ transplants were successfully performed in the 1950s, kidneys have become one of the most commonly transplanted organs in the United States—some 15,000 are performed each year, though demand for the operation far outstrips the availability of donated kidneys. Currently more than 60,000 individuals in the United States are on the waiting list for a kidney transplant.
The operation entails removing a healthy kidney from a live donor or a patient who died with irreversible brain damage and placing it in the lower abdomen of the transplant patient. But that's not the end of the story. As with any "allograft" or transplanted tissue taken from another person, there is still the danger of transplant rejection, which arises from the fact that a donated kidney is foreign to the transplant patient's body.
Left alone, the person's immune system will detect the foreign tissue, mount an immune response, and attack it—acutely "rejecting" or killing the new tissue, leaving the patient no better off than before the transplant. Wishing to avoid transplant rejection, doctors treat patients who have had kidney transplantations with a powerful class of drugs known as immunosuppressants, which weaken the immune response and mitigate the danger. With immunosupressants, a transplanted kidney can survive and function well for years.
However, immunosuppressants also have a dark side. Immunosuppressive drugs make transplant patients more likely to suffer heart disease, diabetes, infections and cancer. These drugs are also toxic, and they can slowly poison the very kidney they are protecting. They can also cause hypertension and hyperlipidemia, eventually leading to the failure of the new kidney transplant—a condition known as chronic allograft nephropathy.
Unlike acute rejection, which is entirely the result of the immune system attacking the transplanted organ, chronic allograft nephropathy may be a result of the immune system, the immunosuppressive drugs, or both. It is a major problem in kidney transplantation, says Salomon, and he points to a recent study from Australia (See: N Engl J Med. Dec 11, 2003, pp. 2326-33) that showed more than half of biopsies taken from kidney transplant patients who appeared to be doing well only two years after transplantation already showed signs of chronic allograft nephropathy. In fact, Salomon recently confirmed these results in his own study of 60 patients on two different types of immunosuppressive drugs and demonstrated that gene expression profiling could be used to define a unique molecular signature for chronic allograft nephropathy.
Because of all the drug toxicities, one of the major challenges in treatment following transplant surgery is to determine the proper regimen of drugs needed for a patient. This is a fine line for doctors to walk. Patients must be given a strong enough dose of the drugs so that their immune systems are kept in check. At the same time, they cannot receive so high a dose that the drugs are toxic to the new kidneys.
Balancing the need for more with the need for less is made more difficult by the fact that every patient responds differently to the immunosuppressant drugs.
It Takes Two to Transplant
In general, says Salomon, if you look at kidney transplant patients a few years after their surgery, they will fall into one of three distinct clinical categories. Some patients will have good kidney function and show no signs of complications or rejection; some will have suffered from acute rejection of their new kidneys within the first few years, and some patients will have chronic allograft nephropathy—but perhaps without any symptoms.
If a patient shows no signs of acute rejection, he/she may be doing perfectly fine. Then again, he/she may be overly immunosuppressed or even headed for chronic allograft nephropathy down the road because of drug-induced kidney toxicity.
"The reality," says Salomon, "is that there is no metric for adequate or safe immunosuppression."
He and his colleagues would like to change that. They would like to use the discoveries of genomic science to build a new set of tools so that doctors can measure and predict how a patient will respond to immunosuppressive drugs. With such tools, transplant doctors could monitor patients regularly to make sure their treatment is always optimal. In fact, these same tools could also guide therapy of patients with diabetes, systemic lupus, rheumatoid arthritis and other immune-related diseases.
The theory is that there may be some genetic "signature" within donors and recipients that predict the best course of treatment following a transplant surgery. This signature could be within the tissues of the transplanted organ or in the blood cells. Salomon and his colleagues want to understand this signature and develop ways to detect it within the laboratory.
They have made progress. In a recent article in the American Journal of Transplantation, Salomon and his colleagues showed for the first time that one could diagnose acute rejection by profiling gene expression in the peripheral blood using high density DNA microarrays. They are now trying to confirm this result in a separate study. A second paper that Salomon published recently showed that they could similarly profile chronic allograft nephropathy in the biopsies of transplanted kidneys.
Now, the NIAID program project grant promises to further the goal by funding a large genomic study of transplant patients. "It is the beginning of applying new technologies to understanding how to diagnose, manage patients, and improve the safety of therapies for organ and cell transplantation," says Salomon.
The grant contains three major projects, all involving the analysis of kidney donors and of patients who have recently undergone kidney transplants.
The grant supports a network of 11 major clinical transplant centers in the United States. "They are doing about 1,400 adult kidney transplants per year and following about 15,000 total patients," says Salomon. The transplantation program at Scripps is one of the clinical centers and Dr. Christopher Marsh, Dr. Caroline Lanigan, biostatistician and Co-Director of the grant's Administrative Core, and Clark Grininger, Informatics Core Manager of the Scripps GCRC, are playing critical roles in developing a secure on-line database to manage the samples and patient information. In the next 5 years, blood and kidney biopsy samples from some 2,400 patients at these centers will be flown to La Jolla to be profiled.
The first project, led by Salomon Steve Head and Sunil Kurian, a post doctoral fellow in Salomon's laboratory, will be looking at the "genomics" of kidney transplantation by profiling the RNA of these patients and their donors. The profiling will be done by extracting the RNA from the samples, labeling it with a fluorescent dye, and placing the fragments on a "gene chip"—a tiny quartz wafer that has thousands of short pieces of DNA attached to it. When applying a sample that contains RNA to the chip, genes present in the sample will "hybridize" or bind to complementary oligonucleotides on the chip. By looking to see which of the oligonucleotides arrayed on the chip have bound the labeled RNA, scientists can measure which genes were being expressed in the sample.
The list of genes expressed in the sample creates the unique profile or signature of the sample discussed above. By comparing the genomic signatures of patients with acute rejection and chronic allograft nephropathy to patients that have never had a rejection and have excellent kidney function, Salomon hopes to develop the knowledge necessary to predict kidney transplant outcome from the signatures.
With this project, Salomon also hopes to gain a better understanding of the basic science of transplantation and to discover which genes in the donor kidney and which genes in the transplant patient are associated with the three clinical outcomes of transplant surgery—acute rejection, normal function, and chronic allograft nephropathy.
The closely-related second project will look at the "proteomics" of kidney transplantation, seeking to identify the proteins important to these three clinical outcomes.
Yates, who is leading the proteomics project, will apply a technology called MudPIT or "shotgun proteomics" that combines liquid chromatography and tandem mass spectrometry to rapidly and sensitively determine the proteins in a complex mixture, such as a sample of biopsy tissue from the kidney transplant or blood cells.
"From these [two projects] we're going to identify 500 gene candidates based on the gene expression and proteomic profiles that are linked to one of three clinical outcomes: acute rejection, chronic allograft nephropathy or long term transplant survival with excellent function," says Salomon.
A third project led by Kwok and Warrington will take these 500 genes and look for single nucleotide polymorphisms (SNPs) within them. SNPs are slight genetic differences among various members of a population. This approach of using the 500 genes identified in the tissue and cell signatures to direct the work of Kwok and Warrington is called "targeted genetics." They will use a new technology called the Mapping 100K Array Set developed by Affymetrix, Inc. (Nasdaq: AFFX) to test all the samples against a set of SNPs chosen to map the whole human genome. This strategy of genome-wide SNP detection is the first step toward a future potential of discovering genes influencing clinical outcomes in medicine.
The end goal will be to identify all the SNPs associated with acute organ rejection and chronic allograft nephropathy, and to develop new SNP chips for all the genes they identify. Such a tool would be helpful to create a profile of patients who have undergone or will undergo kidney transplant surgery to address the genetic matching between the donor and the transplant recipient.
A unique feature of this research effort is that all the genetics will be done on both the patients and their kidney donors. "The genetics of the patient [receiving the kidney] determines the character of the immune response, but it's the genetics of the donor that determines the impact of the transplantation," says Salomon. "What we're hoping to come out with is an understanding of what makes a good donor, and what is it about the donor organ that determines the long-term outcome of the transplant."
Such a tool may also be useful for the development of a new generation of post-transplant drugs to treat patients or to protect the kidneys of patients with early kidney disease that still have good function. The ultimate medical strategy would be to prevent kidney failure and eliminate the need for kidney transplantation. In the meantime, improving the safety of transplantation and increasing the life of the transplants is an important goal.
Send comments to: jasonb@scripps.edu

"What we're hoping to come out with is an understanding of what makes a good [kidney] donor, and what is it about the donor organ that determines the long-term outcome of the transplant," says Associate Professor Daniel Salomon.
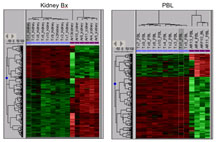
Heat maps provide evidence that gene expression profiling may provide a useful tool for conducting successful kidney transplants. (Click to enlarge.)
LINK:
